🔥 Limited Online Video Consultation Available. Book Your Slot Now | Madinaguda Clinic Mon - Sat : 12 PM - 3 PM | Kukatpally Clinic Mon - Sat : 6 PM - 8 PM
What Is Diabetes? Causes, Symptoms & Management Guide | Dr. Shalini Hyderabad
Comprehensive diabetes guide explaining what diabetes is, why it develops, symptoms to watch for, and evidence-based management strategies. Expert care from Dr. Shalini Patlolla in Hyderabad.
Asian Diabetic Center
7/15/202617 min read
Diabetes: What It Is, Why It Happens, and How It Can Be Managed—A Complete Medical Guide
Diabetes is a long-term medical condition that affects how the body processes sugar and converts food into energy. In India, diabetes affects over 74 million adults—more than any other country except China. Yet despite its prevalence and serious health implications, many people live with diabetes for years without fully understanding how it develops, what it does to their body, or how to manage it effectively.
The misconception: Many people believe diabetes is simply about avoiding sweets or managing weight. The reality: Diabetes is fundamentally about how your body functions every day—how it processes glucose, produces insulin, and how small choices over time impact long-term health outcomes.
At Asian Diabetes Thyroid Hormone Super Speciality Center in Hyderabad, Dr. Shalini Patlolla and her clinical team have educated over 10,000 patients about diabetes pathophysiology and management strategies. This comprehensive guide walks you through the science of diabetes, why it develops, early warning signs, and evidence-based management approaches to help you take control of your health.
Understanding Diabetes: What Happens in Your Body
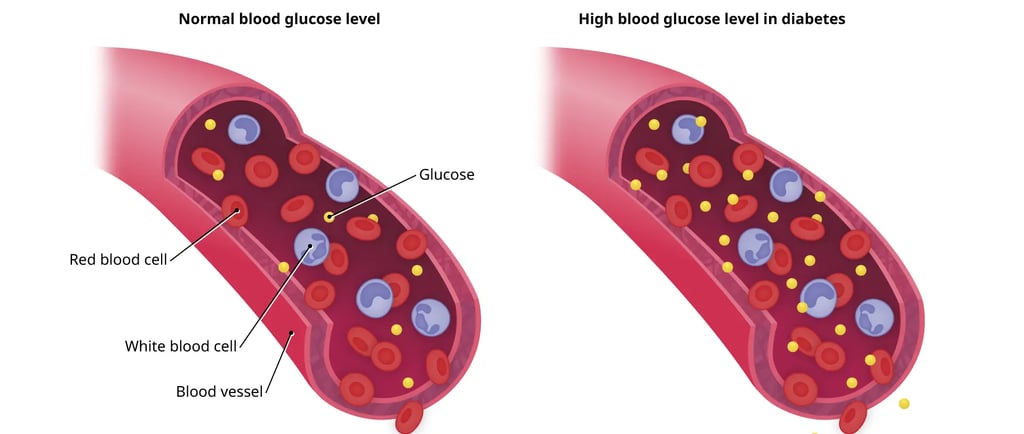
Diabetes occurs when the level of glucose (blood sugar) in the bloodstream becomes higher than normal, leading to a metabolic condition called hyperglycemia. To understand diabetes, you first need to understand how the body normally processes glucose.
The Normal Glucose-Insulin System
Here's how the process normally works in a healthy body:
You eat food containing carbohydrates (bread, rice, fruits, vegetables, sugar)
Digestion begins: Your digestive system breaks down carbohydrates into glucose (the simplest form of sugar)
Glucose enters the bloodstream from the small intestine
The pancreas detects rising blood sugar and responds by releasing the hormone insulin
Insulin acts as a "key": It unlocks cells (muscle, liver, fat cells) so glucose can enter and be used for energy or stored for later use
Blood sugar levels normalize as glucose is utilized or stored
The pancreas reduces insulin production when blood sugar is back to normal—a perfectly calibrated feedback loop
This entire process happens automatically and silently in a healthy person. Blood glucose remains within a narrow, safe range (70-100 mg/dL fasting, less than 140 mg/dL after meals).
What Goes Wrong in Diabetes
In diabetes, this finely-tuned system breaks down in one of two ways:
In Type 1 Diabetes (5-10% of cases):
The immune system mistakenly attacks the insulin-producing beta cells in the pancreas
The pancreas produces little to no insulin
Glucose accumulates in the blood because there's no "key" to unlock cells
This is an autoimmune disease, not caused by diet or lifestyle
Typically develops in children or young adults (though it can occur at any age)
Requires insulin therapy for survival
In Type 2 Diabetes (90% of cases):
The pancreas produces insulin, but the cells become insulin resistant—they don't respond properly to insulin signals
It's like the "lock" on the cell no longer fits the "key" (insulin)
The pancreas initially compensates by producing more insulin, but this is unsustainable
Over time, the pancreas produces less insulin (beta cell dysfunction)
Glucose accumulates in the blood, causing hyperglycemia
Develops gradually, often over years
Can be prevented or delayed with lifestyle changes if caught early
The Progressive Nature of Type 2 Diabetes
Type 2 diabetes typically follows this pattern:
Stage 1: Insulin Resistance (Normal Blood Sugar)
Cells don't respond to insulin properly
Pancreas produces extra insulin to compensate
Blood sugar levels remain normal (for now)
No symptoms
Detectable only through advanced testing (fasting insulin levels, HOMA-IR score)
Stage 2: Prediabetes (Impaired Fasting Glucose)
Pancreas can't keep up with demand
Fasting blood glucose: 100-125 mg/dL (normal is <100)
Cells are getting worse at utilizing glucose
Many people have no symptoms
This stage is reversible with aggressive lifestyle changes or early medication
Stage 3: Type 2 Diabetes (Hyperglycemia)
Fasting blood glucose: ≥126 mg/dL
Symptoms begin to appear
Complications can develop if left uncontrolled
Requires medication in addition to lifestyle changes
Stage 4: Insulin-Requiring Type 2 Diabetes
Pancreatic function continues to decline
Oral medications alone no longer control blood sugar
Insulin therapy becomes necessary
This progression is gradual and natural—not a sign of failure
Why Does Diabetes Happen? Understanding Risk Factors
Diabetes usually develops gradually due to a combination of factors rather than a single cause. It's helpful to think of diabetes risk like a dam—multiple cracks eventually lead to overflow.
Genetic and Hereditary Factors
Genetics play a significant role in diabetes development:
If one parent has Type 2 diabetes: Your risk is approximately 40%
If both parents have Type 2 diabetes: Your risk increases to 70%
If a sibling has Type 2 diabetes: Your risk is elevated
However, genetics is not destiny. Even with strong family history, lifestyle changes can prevent or delay diabetes onset by 5-10 years on average. Conversely, people with no family history can develop Type 2 diabetes due to lifestyle factors.
At our clinic in Madinaguda and KPHB, we work with many families where only one sibling developed diabetes despite identical genetic predisposition—highlighting the importance of lifestyle intervention.
Lifestyle Factors (The Modifiable Risks)
1. Diet Quality and Calories:
Consistently eating high-calorie, high-fat, highly-processed foods contributes to weight gain and insulin resistance
Refined carbohydrates (white bread, sugary drinks, pastries) cause rapid blood sugar spikes, exhausting the pancreas
Lack of fiber means slower glucose absorption, stressing the insulin response system
Portion sizes have increased significantly in the last 30 years (a major contributor to the diabetes epidemic)
2. Physical Inactivity:
Sedentary lifestyle is one of the strongest predictors of Type 2 diabetes development
Muscle cells are the primary consumers of glucose; without muscle activity, glucose accumulates in the blood
Even people at a healthy weight who are sedentary have elevated diabetes risk
Regular physical activity improves insulin sensitivity within days, even before weight loss occurs
3. Excess Body Weight (Especially Abdominal Fat):
Being overweight or obese increases Type 2 diabetes risk by 2-5 times
Abdominal (visceral) fat is particularly problematic—it releases inflammatory chemicals that worsen insulin resistance
However, 10-15% of people with Type 2 diabetes are at a normal or lean body weight, showing that weight is one factor among many
4. Chronic Stress:
Stress hormones (cortisol, adrenaline) increase blood glucose and interfere with insulin production
Chronic stress contributes to weight gain (especially abdominal fat)
Stress impairs sleep quality, which further worsens insulin resistance
High-stress occupations show elevated diabetes rates
5. Sleep Deprivation:
Sleep loss (less than 6 hours nightly) is associated with a 2-3 times increased diabetes risk
Poor sleep disrupts hormones that regulate appetite and glucose metabolism
Sleep apnea (common undiagnosed condition) significantly increases diabetes risk
6. Hormonal Imbalances:
PCOD (Polycystic Ovarian Disease): Up to 50% of women with PCOD develop Type 2 diabetes or prediabetes. Dr. Shalini specializes in PCOD-diabetes connections and offers integrated management at our clinics.
Thyroid disorders: Hypothyroidism slows metabolism; hyperthyroidism can increase insulin resistance
Other hormonal conditions: Cushing's syndrome, acromegaly increase diabetes risk
7. Advancing Age:
Risk increases significantly after age 45 (though Type 2 diabetes increasingly affects younger people)
Age-related decline in insulin production and sensitivity contributes to risk
However, age alone is not the cause—many 70-year-olds have perfect blood sugar control
Other Contributing Factors
Ethnicity: South Asian, African, Hispanic, and Native American populations have 1.5-3x higher Type 2 diabetes prevalence
Gestational diabetes history: Women who developed gestational diabetes during pregnancy have 50% risk of developing Type 2 diabetes later
Inflammatory conditions: Chronic inflammation markers predict diabetes development
Certain medications: Corticosteroids, antipsychotics, some anti-HIV drugs can trigger diabetes
Viral infections: Some viruses may trigger Type 1 diabetes in genetically predisposed individuals
Early Warning Signs: Recognizing Diabetes Symptoms
Diabetes symptoms often develop gradually and can be subtle initially, which is why many people unknowingly live with the condition for years. The average diagnosis delay in India is 2-3 years after symptom onset. Early recognition is crucial because complications develop silently during this undiagnosed period.
Common Early Symptoms
1. Excessive Thirst (Polydipsia) & Frequent Urination (Polyuria)
What's happening: High blood glucose levels exceed the kidney's filtering capacity, causing glucose to spill into urine. This creates an osmotic effect, pulling water with it and causing frequent, excessive urination. The body becomes dehydrated, triggering intense thirst.
What to watch for:
Drinking much more water than usual
Needing to urinate 8-10+ times daily (or multiple times nightly—nocturia)
Waking up 2-3+ times at night to urinate (disrupts sleep quality)
2. Increased Hunger (Polyphagia), Despite Eating Regular Meals
What's happening: Even though you're eating, your cells aren't receiving glucose efficiently (due to insulin resistance). The body perceives this as "starvation" and triggers hunger signals, even after adequate food intake.
What to watch for:
Constant hunger pangs 1-2 hours after eating
Eating more than usual without weight loss (or despite weight loss)
Persistent feeling of dissatisfaction after meals
Cravings for carbohydrates
3. Unusual Fatigue and Lack of Energy
What's happening: Glucose isn't efficiently entering cells for energy production. Your cells are literally "starving" for fuel despite high blood glucose. Additionally, the constant work of managing high blood sugar exhausts the body.
What to watch for:
Persistent tiredness despite adequate sleep
Afternoon energy crashes
Difficulty concentrating at work
Reduced exercise tolerance
Feeling like you're "moving through water"
4. Blurred Vision
What's happening: High blood glucose causes the eye lens to swell, changing its shape and ability to focus. Over time, chronic hyperglycemia damages the tiny blood vessels in the retina (diabetic retinopathy).
What to watch for:
Gradual vision changes (not sudden—that requires emergency evaluation)
Difficulty reading fine print
Blurry distance vision
Floaters or dark spots in vision (sign of more advanced retinopathy)
Important: If you experience sudden vision loss, flashing lights, or large numbers of floaters, seek immediate medical attention—this could indicate retinal hemorrhage.
5. Slow Wound Healing
What's happening: High blood glucose impairs white blood cell function and reduces collagen production, both essential for wound healing. Additionally, diabetes often damages nerves and blood vessels, further compromising healing.
What to watch for:
Paper cuts or minor wounds taking weeks to heal (should take 3-5 days normally)
Increased susceptibility to infections
Small wounds becoming larger or infected
Bruises taking longer to fade
6. Frequent Infections
What's happening: Hyperglycemia weakens the immune system. High blood glucose impairs white blood cell function and creates an environment where bacteria and fungi thrive.
What to watch for:
Recurrent urinary tract infections (UTIs) in women
Fungal infections (oral thrush, vaginal yeast infections)
Skin infections or boils
Frequent colds or respiratory infections
Slow healing of infected wounds
7. Tingling or Numbness in Hands and Feet (Paresthesias)
What's happening: Prolonged hyperglycemia damages the small blood vessels and nerves that supply your hands and feet. This is the early stage of diabetic neuropathy.
What to watch for:
Pins-and-needles sensation in feet (especially at night)
Numbness in toes (difficulty feeling when you step)
Tingling in fingers
Cold feet despite warm weather
Later stages: sharp pain, burning sensations, loss of sensation
8. Unexplained Weight Loss (in Type 1 Diabetes)
What's happening: In Type 1 diabetes, without insulin, the body can't utilize glucose. It breaks down muscle and fat for energy instead, causing rapid weight loss despite normal or increased eating.
This is usually a Type 1 diabetes symptom and requires urgent evaluation.
Asymptomatic Diabetes (The Silent Killer)
Important: Many people have no symptoms at all when diabetes develops. In fact:
Type 2 diabetes is silent: 25% of people are undiagnosed because they have no symptoms
Prediabetes is completely asymptomatic: Most people don't know they're in the danger zone until routine screening
This is why regular health check-ups are crucial, especially if you have risk factors:
Family history of diabetes
Age over 35-40
Overweight or obese
Sedentary lifestyle
PCOD (women)
Gestational diabetes history
High blood pressure or high cholesterol
At our clinic in Hyderabad, we recommend screening every 2-3 years for everyone over 35, and annually for those with risk factors.
What Happens When Diabetes Is Left Uncontrolled?
The damage from uncontrolled diabetes is insidious—it develops silently for years before symptoms appear. Hyperglycemia damages blood vessels and nerves throughout the body through multiple mechanisms:
Oxidative stress: High glucose produces harmful molecules (free radicals) that damage cells
Glycation: Glucose molecules attach to proteins, forming advanced glycation end products (AGEs) that damage tissues
Inflammation: Chronic hyperglycemia triggers inflammatory cascade, accelerating vessel and nerve damage
Endothelial dysfunction: Blood vessel linings become dysfunctional, reducing blood flow and oxygen delivery
Timeline of Complications:
5-10 years: Microangiopathy (small vessel damage) begins silently; early kidney and eye changes detectable on testing
10-15 years: Neuropathy symptoms begin; kidney disease becomes clinically evident
15+ years: Macrovascular (large vessel) complications: heart attacks, strokes become more common; limb amputation risk increases
Long-Term Complications of Uncontrolled Diabetes
Understanding these complications isn't meant to frighten you—it's meant to motivate prevention and early treatment. All of these complications can be prevented or significantly delayed with proper diabetes management.
Cardiovascular Disease (Heart Attacks & Stroke)
The Impact:
People with diabetes are 2-4 times more likely to have a heart attack or stroke
Cardiovascular disease is the #1 cause of death in people with diabetes
Diabetes damages large blood vessels (arteries) causing atherosclerosis
Why It Happens:
Hyperglycemia damages the inner lining of blood vessels (endothelium)
Diabetes accelerates plaque formation in arteries
Blood clotting abnormalities increase stroke risk
Diabetes often coexists with high blood pressure and high cholesterol (the "perfect storm")
Prevention at Our Clinic:
Regular cardiac risk assessment (lipid panel, blood pressure monitoring)
ECG screening for asymptomatic disease
Lifestyle counseling focused on heart health
Medication optimization to reduce cardiovascular risk
Diabetic Kidney Disease (Diabetic Nephropathy)
The Impact:
Approximately 40% of people with diabetes develop kidney disease
Diabetes is the leading cause of kidney failure requiring dialysis in India
Early stages are silent (no symptoms until significant damage)
Why It Happens:
Hyperglycemia damages the filtration units in the kidneys (glomeruli)
High blood pressure accelerates kidney damage
Protein begins leaking into urine (first sign of damage)
Gradually, kidney function declines
Detection & Prevention at Our Clinic:
Annual screening: Urine microalbumin test (detects early kidney damage)
Regular lab work: Creatinine and GFR (Glomerular Filtration Rate) assessment
Blood pressure management: Critical for slowing progression
Medications: ACE inhibitors or ARBs reduce kidney damage progression
Dietary management: Protein and salt intake optimization
Diabetic Nerve Damage (Diabetic Neuropathy)
The Impact:
Affects approximately 50% of people with diabetes (many unaware)
Can progress from tingling to complete loss of sensation
Increases amputation risk through undetected injuries
Causes significant pain in some cases
Types:
Peripheral Neuropathy (Most Common):
Affects feet and hands
Early: tingling, numbness
Later: burning pain or complete loss of sensation
Increases injury risk (ulcers, infections)
Autonomic Neuropathy:
Affects internal organs
Causes: sexual dysfunction, digestive problems, blood pressure irregularities, impaired sweat response, heart rhythm abnormalities
Why It Happens:
Hyperglycemia damages nerve cell insulation (myelin)
Reduced blood flow to nerves
Accumulation of sorbitol in nerve cells
Prevention & Management at Our Clinic:
Early detection: Monofilament testing, vibratory sensation testing
Tight glucose control: Slows progression
Vitamin supplementation: B vitamins support nerve health
Specialized foot care: Crucial for preventing complications
Diabetic Eye Disease (Diabetic Retinopathy)
The Impact:
Leading cause of blindness in working-age adults
Approximately 25% of people with 15+ years of diabetes develop retinopathy
Often has no symptoms until significant damage
How It Develops:
Stage 1: Nonproliferative Retinopathy: Small blood vessel damage, microaneurysms, fluid leakage
Stage 2: Proliferative Retinopathy: New abnormal blood vessels form, increasing bleed risk and vision loss risk
Prevention & Detection at Our Clinic:
Annual dilated eye exams: Essential for early detection
Referral to ophthalmologist: If abnormalities detected
Laser treatment: Can halt progression if caught early
Glucose control: Primary prevention strategy
Blood pressure management: Critical for slowing progression
Diabetic Foot Problems (Including Amputations)
The Impact:
Diabetes is the leading cause of non-traumatic limb amputation
Minor foot injuries can progress to amputation if untreated
Often preventable with proper care
How It Develops:
Neuropathy: Loss of sensation means injuries go unnoticed
Poor circulation: Reduced blood flow delays healing
Infection risk: Infection from unnoticed wounds spreads quickly
Example cascade: Small blister → unnoticed due to neuropathy → becomes infected → ulcer develops → infection spreads → amputation required
Prevention & Care at Our Clinic:
Specialized diabetic foot screening: Regular assessments
Neuropathy assessment: Monofilament testing
Circulation testing: Doppler ultrasound if needed
Foot care education: Proper daily care techniques
Custom footwear recommendations: Reduces pressure ulcer risk
Wound care expertise: Prevents minor issues from escalating
Early referral: To vascular surgeons if circulation compromised
Other Complications
Skin Infections:
Diabetic patients are prone to bacterial and fungal skin infections
Infections spread more easily due to impaired immunity
Hearing Loss:
Diabetes accelerates age-related hearing loss
Mechanism: nerve damage affects the inner ear
Dental Disease:
Hyperglycemia impairs white blood cell function
Gum disease develops faster and is more severe
Infections are harder to control
Mental Health Issues:
Depression is 2-3 times more common in people with diabetes
Diabetes distress, anxiety, and adjustment disorders are significant
Cognitive Decline:
Chronic hyperglycemia is linked to increased dementia risk
Vascular damage affects brain blood vessel health
Solutions and Treatment Options: Managing Diabetes Effectively
Managing diabetes requires consistency rather than extreme measures. The good news: Diabetes can be effectively controlled with the right approach, preventing or significantly delaying complications. Successful management combines three pillars: lifestyle modification, medication when needed, and regular monitoring.
Pillar 1: Lifestyle Modification (The Foundation)
Nutrition: Medical Nutrition Therapy (MNT)
Proper nutrition is the cornerstone of diabetes management. This isn't about deprivation—it's about making informed choices that support stable blood sugar.
Key Principles:
Carbohydrate Quality Over Quantity
Choose whole grains (brown rice, oats, whole wheat bread) over refined carbohydrates
Include fiber: slows glucose absorption, reduces blood sugar spikes
Target 25-30g fiber daily
Include low-glycemic vegetables (leafy greens, broccoli, bell peppers)
Balanced Macronutrients
Include protein at each meal: slows glucose absorption, increases satiety
Choose healthy fats (olive oil, nuts, fatty fish) over saturated fats
Avoid trans fats completely
Portion Control
Use the plate method: ½ plate non-starchy vegetables, ¼ plate protein, ¼ plate whole grains
Avoid large portion sizes even of healthy foods
Pay attention to hunger and fullness cues
Indian Meal Planning for Diabetes
Incorporate traditional foods mindfully
Swap white rice for brown rice or millet
Include dal (high in fiber and protein)
Choose roti over naan (lower fat)
Prepare curries with minimal oil
Include seasonal vegetables
Limit fried foods, sweets, and sugary beverages
Meal Timing
Avoid long gaps between meals (every 3-4 hours)
Eat balanced breakfast to prevent afternoon blood sugar crashes
Avoid eating large meals late at night
At our clinic, our nutritionist works with you to develop a personalized meal plan that fits your lifestyle, preferences, and cultural food habits—not a generic "diabetes diet."
Physical Activity: Exercise & Movement
Physical activity is medicine for diabetes. Exercise improves insulin sensitivity within days—even before weight loss occurs.
Recommended Activity Plan:
Aerobic exercise: 150 minutes weekly (brisk walking, cycling, swimming)
Resistance training: 2-3 sessions weekly (builds muscle, improves glucose utilization)
Flexibility: Daily stretching or yoga
Reduce sedentary time: Break up sitting with movement every 30 minutes
Benefits of Exercise:
Muscles consume glucose without needing insulin (bypasses the resistance problem)
Improves insulin sensitivity
Aids weight loss
Reduces blood pressure and cholesterol
Improves mental health and mood
Reduces cardiovascular disease risk
Indian Exercise Options:
Walking (Madinaguda and KPHB areas have good walking routes)
Yoga (excellent for diabetes; focus on active styles)
Swimming
Cycling
Dance classes
Cricket, badminton, or other sports
Weight Management (If Overweight)
Even modest weight loss (5-10% of body weight) significantly improves insulin sensitivity and blood sugar control.
Set realistic goals (0.5-1 lb per week)
Combine diet and exercise
Address emotional eating patterns
Consider behavioral modification programs
At our clinic, we assess individual weight loss needs and provide ongoing support
Stress Management
Chronic stress elevates cortisol, which increases blood glucose and interferes with diabetes control.
Meditation or mindfulness: 10-15 minutes daily
Deep breathing exercises: Activates parasympathetic nervous system
Adequate sleep: 7-9 hours nightly
Yoga: Combines physical activity with stress reduction
Hobbies and relaxation: Important for psychological well-being
Professional counseling: If depression or anxiety present
Pillar 2: Medical Management (When Needed)
Important: Lifestyle changes alone control blood sugar in some people, but many require medication. Taking medication is not failure—it's successful disease management.
Oral Medications for Type 2 Diabetes:
The goal is choosing the right medication based on your individual needs, other health conditions, and side effect profile.
Common Medication Classes:
Metformin (First-Line Agent)
Reduces liver glucose production and improves insulin sensitivity
Generally well-tolerated
May cause GI side effects initially
Does not cause weight gain; may cause modest weight loss
GLP-1 Receptor Agonists (e.g., Ozempic, Saxenda)
Improves insulin secretion and reduces appetite
Significant weight loss benefits (5-10% body weight)
Injectable once weekly
Well-tolerated; some nausea initially
Lower hypoglycemia risk
SGLT2 Inhibitors (e.g., Dapagliflozin, Empagliflozin)
Causes glucose excretion in urine
Cardiovascular and kidney-protective benefits
Aids weight loss
Generally well-tolerated
Rare but serious UTI risk
DPP-4 Inhibitors (Sitagliptin, Linagliptin)
Improves insulin secretion based on glucose levels
Minimal weight gain or loss
Low hypoglycemia risk
Sulfonylureas (Glibenclamide, Gliclazide)
Increases insulin secretion
Effective but may cause weight gain and hypoglycemia
Now used as second or third-line agents
Thiazoslidinediones (Pioglitazone)
Improves insulin sensitivity
May cause weight gain and fluid retention
Less commonly used now
Insulin Therapy for Type 2 Diabetes:
As discussed in our previous blog, insulin therapy is a natural progression for many patients, not a sign of failure.
Basal insulin: Long-acting insulin once daily at night
Insulin combinations: Rapid-acting insulin with meals + basal insulin
Insulin pumps: Continuous insulin infusion (excellent for some patients)
Modern insulin pens: Make administration easier and more discreet
Type 1 Diabetes Management:
Type 1 diabetes always requires insulin therapy. Modern management includes:
Multiple daily injections (basal + bolus)
Insulin pump therapy
Continuous glucose monitors (CGMs)
Carbohydrate counting and dose adjustments
Pillar 3: Regular Monitoring & Testing
Monitoring is crucial for several reasons:
Guides treatment adjustments
Detects emerging complications early
Provides motivation for lifestyle changes
Identifies barriers to control
Essential Tests at Regular Intervals:
HbA1c (Glycated Hemoglobin) – Every 3 Months
Measures average blood sugar over 3 months
Target: <7% for most patients (can be individualized)
Reflects long-term control and complication risk
Fasting Blood Glucose – Every 3-6 Months
Measures fasting blood sugar
Target: 80-130 mg/dL for most patients
Guides medication adjustments
Home Blood Glucose Monitoring (If on Insulin or Certain Medications)
Tests 1-4 times daily depending on regimen
Helps identify patterns and adjust treatment
Continuous Glucose Monitoring (CGM)
Wearable device measuring glucose every 5 minutes
Excellent for Type 1 diabetes and insulin-requiring Type 2
Provides comprehensive glucose patterns
Increasingly available and affordable
Available at our clinic in Hyderabad
Annual Screening Tests:
Lipid Panel: Cholesterol, triglycerides (manage cardiovascular risk)
Kidney Function: Creatinine, GFR, urine microalbumin (detect early kidney disease)
Liver Function: Assess medication tolerability
Thyroid Function: Screen for thyroid disorders (common with diabetes)
Diabetic Retinopathy Screening: Annual dilated eye exam
Neuropathy Screening: Monofilament test, vibration sense
Foot Examination: Assess circulation, sensation, skin integrity
Blood Pressure Monitoring: Regular checks to control cardiovascular risk
Uric Acid: Elevated levels increase gout and cardiovascular risk
At Asian Diabetes Thyroid Hormone Super Speciality Center, we provide:
Comprehensive annual diabetes screening package
Advanced testing for early complication detection
Continuous glucose monitoring systems
Direct referral relationships with ophthalmologists and nephrologists for specialized care
Additional Considerations: Managing Related Conditions
Diabetes often coexists with other conditions that compound complications. Comprehensive diabetes care addresses these:
Thyroid Disease:
10-15% of people with diabetes develop thyroid disorders (especially Type 1)
Hypothyroidism worsens diabetes control
Dr. Shalini specializes in integrated diabetes-thyroid management at our Madinaguda and KPHB clinics
PCOD (Polycystic Ovarian Disease) in Women:
Affects 20-25% of women of reproductive age
Directly increases insulin resistance and Type 2 diabetes risk
Requires specialized management combining endocrinology and gynecology approaches
Our clinic provides integrated PCOD-diabetes care
Hypertension (High Blood Pressure):
Present in 50-60% of people with diabetes
Dramatically increases cardiovascular and kidney disease risk
Requires aggressive control (<130/80 mmHg target)
Dyslipidemia (Abnormal Cholesterol/Triglycerides):
Common in diabetes
Increases cardiovascular risk
Requires medication in addition to lifestyle changes
Obesity:
Addressed through comprehensive weight management
Bariatric surgery may be considered for severe obesity with inadequate diabetes control
Living Well With Diabetes: Beyond Blood Sugar Numbers
Being diagnosed with diabetes can feel overwhelming initially. You may feel scared, angry, or depressed. These emotions are normal. However, diabetes does not mean life has to be restricted.
Practical Management Strategies
Building Sustainable Habits
Rather than dramatic overhauls, focus on small, sustainable changes:
Add one vegetable to each meal (rather than eliminating foods)
Take a 10-minute walk daily (rather than committing to extreme exercise)
Replace one sugary drink with water
Gradually replace white rice with brown rice
Practice one stress-management technique daily
Support Systems
Family involvement: Share your dietary and exercise goals with family
Diabetes education programs: Learn from certified educators
Peer support groups: Connect with others managing diabetes
Mental health support: If struggling with depression or anxiety related to diagnosis
Mindset Shift
Reframe diabetes: Not a punishment but a condition you can manage
Celebrate wins: Track improvements in energy, mood, and blood sugar control
Practice self-compassion: You'll have off days; this is normal
Long-term thinking: Focus on preventing complications and living well, not perfection
Realistic Expectations
With proper management, people with diabetes can:
✓ Travel and eat out regularly
✓ Participate in sports and exercise
✓ Enjoy occasional treats in moderation
✓ Work in any field (with reasonable accommodations if needed)
✓ Have healthy relationships and families
✓ Live full, active, and healthy lives
What changes:
Greater awareness of food choices
Regular health monitoring
Daily medication (for most)
Lifestyle habits that support health
Frequently Asked Questions About Diabetes
Q: Can diabetes go away or be cured?
A: Type 1 diabetes cannot be cured—it requires lifelong insulin therapy. Type 2 diabetes cannot be cured, but remission is possible. Remission (where blood sugar returns to non-diabetic range without medication) occurs in approximately 10-15% of people with Type 2 diabetes through significant weight loss (typically 15+ kg) and sustained lifestyle changes. The earlier you intervene, the more likely remission becomes possible. Our diabetes reversal program at the clinic focuses on achieving remission through comprehensive lifestyle modification and individualized medical management.
Q: How often should I check my blood sugar?
A: Frequency depends on your diabetes type and treatment:
Type 1 diabetes: 4+ times daily (before meals, bedtime, before/after exercise)
Type 2 on insulin: 2-4 times daily based on your regimen
Type 2 on oral medications: 1-2 times daily or as directed by your doctor
Using CGM: Continuous monitoring (no need for routine finger-stick testing)
At our clinic, we individualize monitoring recommendations based on your specific situation.
Q: Will I need insulin eventually?
A: Not everyone with Type 2 diabetes will need insulin. However, it's a possibility as the disease progresses. Starting insulin when indicated is not failure—it's appropriate medical management. Some patients manage well with oral medications and lifestyle changes throughout their lives.
Q: What should I do if my blood sugar is too high or too low?
A: High blood sugar (>250 mg/dL):
Drink water
Physical activity (if safe)
Take medication as prescribed
Contact your doctor if persistently elevated
Low blood sugar (<70 mg/dL):
Consume fast-acting carbohydrate: 15g glucose (glucose tablets, regular soda, honey)
Recheck in 15 minutes
Eat balanced meal when normal
Consult doctor if frequent lows
Severe hypoglycemia (confusion, seizures, loss of consciousness):
Requires emergency medical care
Glucagon injection (if available and someone knows how to use it)
Call emergency services
Q: Can I get pregnant if I have diabetes?
A: Yes! Women with diabetes can have healthy pregnancies. However:
Pre-conception planning: Critical for optimizing blood sugar control
Tight glucose control: Essential for reducing birth defects and complications
Close monitoring: More frequent prenatal visits and testing
Medication adjustments: Some diabetes medications are unsafe in pregnancy; insulin is preferred
Gestational diabetes: Women with Type 2 diabetes planning pregnancy should consult a diabetes specialist
Our clinic provides comprehensive pre-conception and pregnancy counseling for women with diabetes.
Q: How does illness or stress affect my blood sugar?
A: Both illness and stress elevate stress hormones that increase blood glucose:
During illness, blood sugar often rises even if you're eating less
Contact your doctor for guidance on medication adjustments
Continue taking diabetes medications unless directed otherwise
Stay hydrated
Monitor blood sugar more frequently
Mental/emotional stress similarly elevates blood glucose—stress management becomes more important during stressful periods
Q: Is it safe to exercise with diabetes?
A: Yes! Exercise is beneficial for diabetes management. However:
Check blood glucose before exercising (especially if on insulin)
Carry fast-acting carbohydrates
Stay hydrated
Avoid exercising at times of peak medication action
Wear identification indicating you have diabetes
Inform exercise partners/trainers about your condition
Our clinic can provide exercise recommendations tailored to your fitness level and diabetes regimen.
Q: Can I manage diabetes without taking medications?
A: Some people with Type 2 diabetes can achieve adequate blood sugar control through lifestyle changes alone, especially if diagnosed early. However, many require medications. Taking medication is not a sign of failure—it's appropriate disease management. Type 1 diabetes always requires insulin.
Q: What lifestyle changes have the biggest impact on blood sugar?
A: In order of impact:
Weight loss (if overweight) – 5-10% loss significantly improves insulin sensitivity
Regular physical activity – Improves insulin sensitivity within days
Diet quality – Reducing refined carbohydrates and increasing fiber
Sleep quality – 7-9 hours nightly supports glucose regulation
Stress management – Reduces cortisol-induced blood sugar elevation
All five work together synergistically.
Final Thoughts: Taking Control of Your Diabetes
Diabetes is a condition that requires awareness, patience, and ongoing care—not fear. Understanding what diabetes is, why it develops, and how it affects your body empowers you to take control of your health. You are not powerless in the face of this diagnosis.
Key Takeaways:
Diabetes develops gradually, often over years—early intervention during prediabetes or early Type 2 diabetes stages can prevent progression or achieve remission
Lifestyle changes are powerful medicine—diet, exercise, stress management, and sleep have profound effects on blood sugar control
Medications are tools, not punishments—they're used when needed to achieve healthy blood sugar levels
Regular monitoring and screening are essential—early detection of complications prevents progression
Complications are preventable—with proper diabetes management, most serious complications can be avoided or significantly delayed
You can live well with diabetes—thousands of our patients at the clinic lead full, active, healthy lives while managing diabetes effectively
Quick Links
Dr. Shalini Patlolla is a best endocrinologist and diabetologist in Madinaguda and Kukatpally, Hyderabad, providing expert care for diabetes, thyroid disorders, PCOD/PCOS, and all hormonal problems. Book your online consultation with Dr. Shalini today for advanced endocrine and diabetes treatment in Hyderabad.
Email ID - drshaliniendocrine@gmail.com
Follow Us :
Walk-In
Madinaguda Clinic Address
H. No. 7-1/2, Above New Reliance Car Decors, Opp. Bharat Petroleum, Sri Durga Colony, Madinaguda Main Road, Hyderabad - 500050
Opening Hours :
Mon - Sat: 12 PM - 3 PM
Kukatpally Clinic Address
MID-286, Opp. Global Edge School, Road No. 4, Remedy Hospital Lane, KPHB Colony, Hyderabad - 500072
Opening Hours :
Mon - Sat: 6 PM - 8 PM
Designed by Harshming Web services © 2025. All rights reserved.
Contact Number- +91-9133552279


